
HEALTH specialists and advocates across the region said there were "no surprises" in the damning findings from an inquiry into medical care in regional, rural and remote NSW.
Subscribe now for unlimited access.
or signup to continue reading
The report, tabled in state parliament on Thursday, was the result of a year-long inquiry receiving 720 submissions and 15 hearings.
As a result of the findings, the upper house report made 44 recommendations, including an urgent review of the rural workforce and funding arrangements, along with better engagement with rural communities.
ALSO MAKING NEWS:
- Shop owner threatened with sauce bottle for asking man to wear a mask
- School children's safety the priority for Dubbo Mayor Mathew Dickerson
- Truck driver who killed two people appeals conviction claiming 'miscarriage of justice'
- Outpouring of help for local couple trying to raise money for their wedding
'No simple solution'
Significant attention and intervention is needed to fix rural and regional health services, says a Dubbo psychologist.
Psychologist and founder of the Macquarie Health Collective Dr Tanya Forster said that she was pleased to see that rural health services would be receiving attention after the release of the inquiry's findings, especially with a federal election approaching.
"This is a long standing issue, with no simple solution, but it is an issue that deserves significant attention and intervention," she told Daily Liberal.
She also said that the regional health inquiry's latest report was an important step in the right direction, but it was more important to see measures implemented in the concerned areas.
"322 pages of consultation and research is great, as long as it leads to action," she said.
The report involved multiple components like improving the number of health professionals in regional areas, improving culturally appropriate care for First Nations people, a review of the nursing and midwifery workforce, and establishment of a palliative care taskforce, to name a few. Dr Forster stated that it would require efforts from multiple directions and collaboration between different levels of government.
As a local health service leader, she was well aware of the issues and the impact on healthcare, but according to her, there is no one person or one organisation at fault here.
"This is a complex issue. This is not about blame, but it is about change," she said.
Dr Forster wants to see changes in the way rural health services are funded and believes "we need to rethink the way we recruit to regional areas".
"We need to change the way we talk about and teach regional health, from the moment a person commences their first day of university, to the moment they retire."
Most of all, she says we need to start to change the way we talk about regional Australia.
"Every person can play a role in that," she said.
She hopes that with the new report, change will follow.
Report confirms what we already know
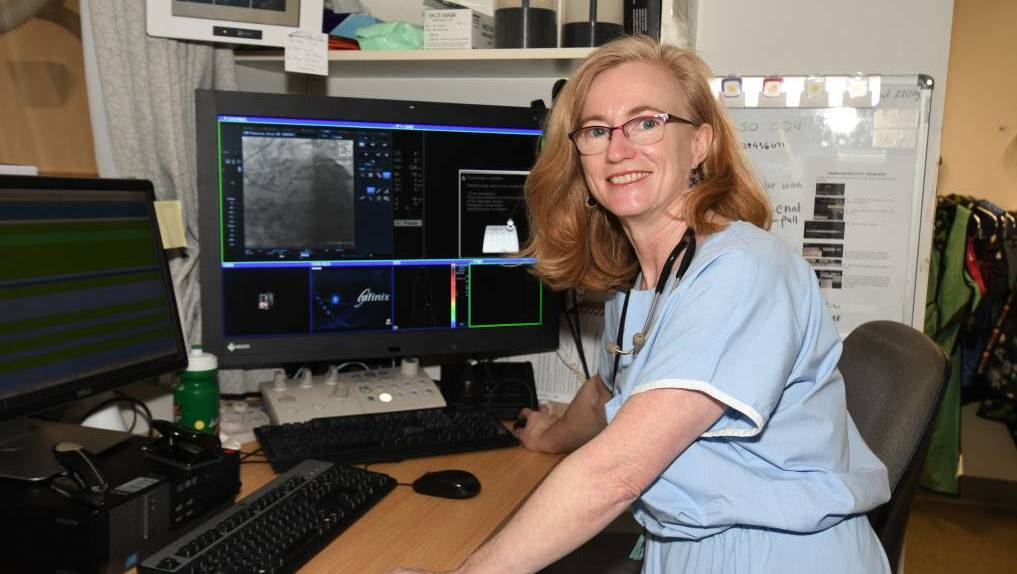
Dr Ruth Arnold, a cardiologist based in Orange, was among those to put in a submission and appear before the inquiry, where she was critical of telehealth staffing and the fear of retribution on speaking out against the system.
She said on Friday the report simply confirmed what those working in the health system already know.
"That is that our current health system is not good enough in regional and rural areas, let's just be blunt," she said.
"There are a lot of deficiencies and I think the report has confirmed those.
"What we need to do now is take up some of those recommendations and make this better."
She said while the report made some good recommendations, they must be followed through.
"It's a federal and state issue in no uncertain terms and it will not be fixed in rural and regional areas without a complete overhaul of the federal and state model,' she said.
Reflects the issues already raised
Bathurst Regional Councillor Warren Aubin, who is part of the city's Health Services Action Group, said the findings and recommendations detailed in the report reflect the issues that were raised about health services in Bathurst.
The inquiry had 22 findings. Among them includes:
- That rural, regional and remote patients have significantly poorer health outcomes, greater incidents of chronic disease and greater premature deaths when compared to their counterparts in metropolitan areas.
- That residents in rural, regional and remote New South Wales have inferior access to health and hospital services, especially for those living in remote towns and locations and Indigenous communities, which has led to instances of patients receiving substandard levels of care.
- That residents living in rural, regional and remote communities face significant financial challenges in order to access diagnosis, treatment and other health services compared to those living in metropolitan cities.
- That rural, regional and remote medical staff are significantly under resourced when compared with their metropolitan counterparts, exacerbating health inequities.
- That there is a critical shortage of health professionals across rural, regional and remote communities resulting in staffing deficiencies in hospitals and health services.
- That there has been a historic failure by various NSW and Australian governments to attract, support and retain health professionals especially doctors and nurses in rural, regional and remote areas.
- That there is a culture of fear operating within NSW Health in relation to employees speaking out and raising concerns and issues about patient safety, staff welfare and inadequate resources.
No comment from Western NSW Local Health District
The Western NSW Local Health District has refused to comment on the findings.
Australian Community Media reached out to the local health service to find out what would be done now the findings have been released.
However, a spokesperson said because it was based on regional and rural areas statewide it was more appropriate for NSW Health or Regional Health Minister Bronnie Taylor to respond.
The WNSWLHD was asked about what the most pressing concerns were following the inquiry and whether it would result in meaningful change.
It was also asked if there was confidence the inquiry would result in meaningful change, and what steps were being taken to improve transparency among health services.


