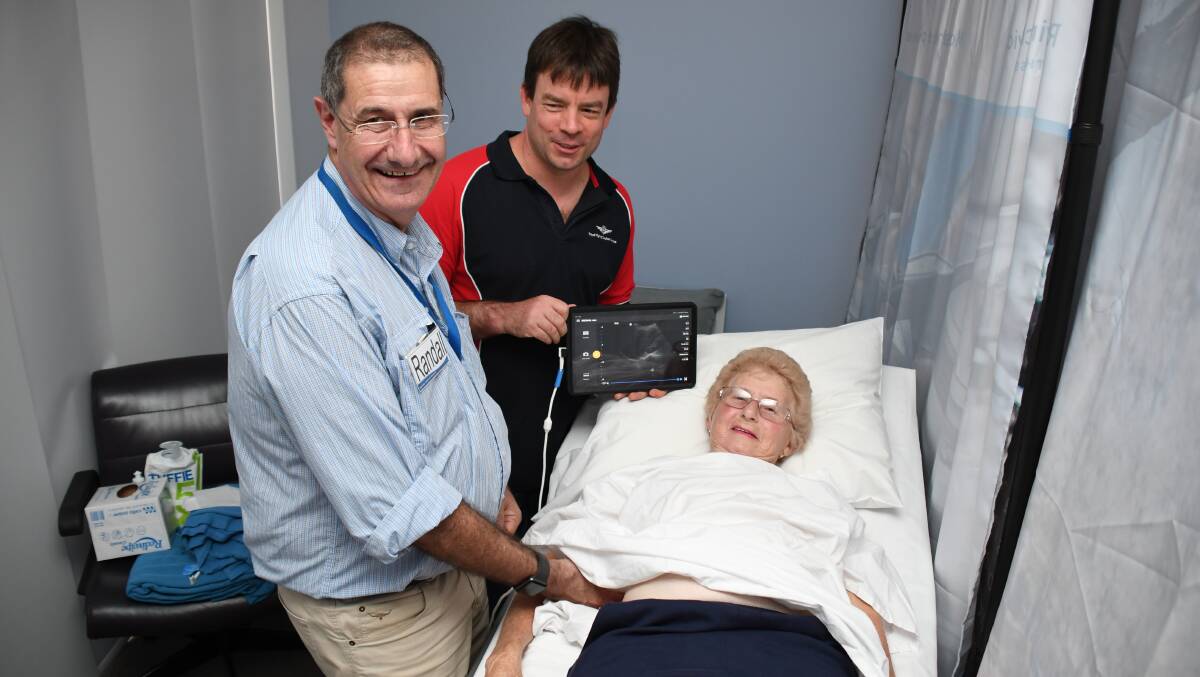
Dubbo's Garry Taylor was staying mum about his open heart and bowel operations as he prepared to be scanned at the Royal Flying Doctor Service (RFDS) Dubbo Base on Tuesday.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
He wanted to give the base's medical officers the opportunity to discover his surgical journey by themselves.
Mr Taylor is among more than 40 members of the public who have gladly volunteered to be scanned during three days of ultrasound training.
He wasn't giving anything away as he arrived at the base, except the reason why he was lending a hand.
"The RFDS..you can't beat them," he said.
In late February the RFDS put out a call for volunteers to help the base's medical officers build on their ability to use ultrasound equipment.
The base had acquired new transportable ultrasound gear, essentially two Android tablets with probes, costing about $60,000.
Dr Peter Brendt, emergency services team leader for the RFDS South Eastern Section, was concerned that getting the equipment would be far easier than arranging training.
When two sonographers from the Australian Institute of Ultrasound were on board, he looked to the community.
"Every hour we have three volunteers," he said on Tuesday, day two of the training.
"Dubbo has been really generous with us."
"It shows really great community spirit to come in and help us."
Both doctors and flight nurses are involved in the training which focused on emergency scanning procedures.
"Everybody in the team needs to be able to use our equipment," Dr Brendt said.
"If you work in our area you just have to do what needs to be done."
Dr Brendt said the transportable ultrasound equipment would be on "every aircraft which goes out to a critical job".
"If you have a trauma patient you want to know if they are bleeding into the chest or the belly," he said.
"You might start to give some blood transfusions then or work on getting them to the right place."
Dr Brendt said the new equipment would enable early diagnosis of a ruptured aortic aneurysm allowing for the transfer to the "right surgeon" for life-saving treatment.
It would also make the insertion of a cannula more precise through observation of blood vessels.
Dr Brendt predicts ultrasound equipment will get cheaper, smaller and more portable.
"In the past a doctor was known because he had a stethoscope around his neck," he said.
"I would imagine in the future it's just having an ultrasound probe in your hand."

